Consultant (Doctor) Worship
I raised this on my agenda in supervision once ‘Consultant (doctor) worship’. And the response from my supervisor: ‘I’m intrigued already…’
So what do I mean by this? Well it never ceases to amaze me in particular health services, how the view of Doctor as GOD still lives on. I’ve actually seen a colleague curtsey to a doctor once. I’ve seen another colleague ask the doctor how she should plan her (occupational therapy services). Very inappropriate (doctors don’t know everything). And the pressure must be huge.
I’ve also had colleagues whispering behind the doctor’s back ‘oh… we mustn’t be late to ward round as the doctor doesn’t like it’.
I wonder if they hear themselves let alone ‘see’ what they look like and how it comes across when they behave in such a way; it’s a little like children afraid of Mum or Dad. Yet we’re actually all adults working together in the care of clients/ patients. And deserve equal respect as such. I’d like an environment where doctors can also feel able to ask for help or say when they don’t know something.
The thing is a Doctor / Consultant is a person. Although they are often charged with being the Clinical team leaders, this does not necessarily mean that they are best placed to fulfil this role (or even want it). There is in healthcare a long standing stereotype of doctor as ‘stuffy’ and unapproachable. Well what good is this, if we are all colleagues and we require to work effectively in the spirit of teamwork? We must ask if they have been trained sufficiently to adequately fulfil the role of leader? Have they completed any management or leadership training? How well did they do in this training? What is their self-leadership skills like? These are all highly relevant questions because a leader who is poorly skilled will lead his or her team poorly and we have plenty of examples in recent press of where this has happened in NHS institutions. and many other institutions too, this is explored in this blog.
Also, doctors and consultants, especially in mental health, often have the least contact with clients; it is typically the occupational therapists (or rehabilitation team) that have a lot of qualitative time with clients through provision of therapeutic group activities, 1-1 interventions and rehabilitation programmes. So it could be argued that it would make better sense for these professionals to be the team leads?
A subtle shake-up
It’s all a matter of perspective really. The NHS is run from an entrenched and outdated hierarchial and patriarchial medical model. So it would make sense that the leaders are therefore the doctors in the current system. But with many health institutions recognising a more recovery based model, it follows that the leaders would change to follow suit.
Challenging models of hierarchy
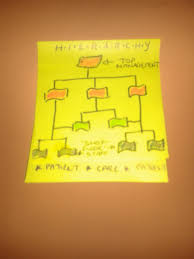
In my experience, this is the typical model of hierarchy in the NHS and most institutions. Normally the manager is at the top of the hierarchy and supervises the person below, and the pattern flows down.
I often think that it would be useful to flip this, so that the roles are reversed and the managers are at the bottom of the hierarchy; for we can learn so much from those we manage.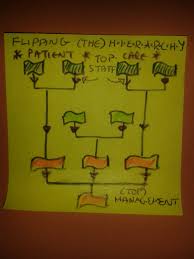
For how often do we get asked to rate our managers’ competence? Afterall we would know, wouldn’t we? Who else is better positioned to rate their manager’s skills than the persons whom they manage?
It could be incorporated within PDPs (Personal Development Plans) to capture this very worthwhile information which is otherwise a lost resource. I think the diagrams provide much useful food for thought; we can see that shop floor staff are closest to patients and so knowledge about patient care ad needs would aturally flow down the chain as indicated. However we know that this is not the way it works.
Advantages to flipping the hierarchy
- Managers leading and being able to manage their teams more effectively.
- Managers getting to know their staff and colleagues better.
- Managers having a clearer idea about what their supervisees / staff want and need from their manager.
Lastly, I think this Guardian article about ‘The ten essential qualities of leadership in the NHS’ raises some useful points for consideration.